The functional medicine approach to autoimmune remission focuses on restoring balance by addressing root causes such as gut health, chronic inflammation, nutrient gaps, and daily habits. Instead of only easing symptoms, this method looks at how the body’s systems connect and affect one another.
With this perspective, care becomes more tailored, more precise, and often more sustainable. The process usually begins with detailed testing and a plan designed for your unique health history and needs. Keep reading to learn the key steps and principles behind this approach.
Key Takeaways
- Functional medicine looks for the root causes of autoimmune issues, aiming for lasting health instead of short-term symptom control.
- A personalized care plan that includes thorough testing and lifestyle changes can strongly improve outcomes for people with autoimmune conditions.
- Supporting and healing the gut is central to balancing the immune system and maintaining long-term remission.
Functional Medicine Approach to Autoimmune Remission
What Does a Functional Medicine Approach Mean for Autoimmune Remission?
In functional medicine, remission is pursued by looking at root causes rather than only calming flares. This philosophy is grounded in Functional Medicine Care & Integrative Foundations, which emphasize how gut health, food sensitivities, nutrient status, stress, sleep, movement, and daily habits quietly shape immune behavior. The Institute for Functional Medicine notes that roughly 80% of the immune system is influenced by the gut, making digestion and microbiome balance central to care.
Instead of relying only on medications to suppress the immune response, practitioners look for what might be driving it. That can include dietary triggers, chronic infections, environmental toxins, blood sugar swings, or hormonal imbalances. These areas are evaluated through a combination of history-taking, targeted lab testing, and close tracking of symptoms over time.
By addressing these drivers, the goal is to calm the immune system from the inside out. Protocols are then tailored to the individual, two people with the same diagnosis may have very different plans. Over time, many patients experience fewer flares, better resilience, and a clearer path toward sustained remission rather than short-term relief.
How Remission Is Defined Beyond Symptom Control
In functional medicine, remission is not defined only by symptom reduction, even though symptoms matter. A more complete picture is often built through functional medicine services for personalized healing that track both clinical and lifestyle markers over time.
- Lab markers (such as inflammation levels or organ-specific markers)
- Frequency and intensity of symptom flares
- Medication needs and dosage changes
- Daily function and quality of life
Patients may notice they can do more with less fatigue, sleep more soundly, think more clearly, and handle stress without immediate flare-ups. These shifts, combined with improved lab markers and reduced reliance on medications when appropriate and safe, suggest deeper change rather than surface-level control.
This perspective differs from many conventional approaches that focus mainly on symptom reduction and disease control. Functional medicine works alongside necessary medical treatments but aims to change the terrain that allowed autoimmunity to develop or worsen. The focus is on long-term stability, less inflammation, and a body that is supported to stay in remission, not just managed during flares.
How Is Remission Assessed with Comprehensive Functional Testing?
When someone is working toward autoimmune remission, testing becomes less about chasing numbers and more about understanding what the body is trying to say. Functional medicine uses comprehensive testing to build a clear picture of what is driving the immune system out of balance.
The testing plan is usually tailored to the person, not just the diagnosis. These assessments can look at gut health, inflammation, nutrient status, hormones, and possible toxin exposure. Together, they help guide a more focused and realistic plan for remission, rather than guessing or using a one-size-fits-all approach.
Core Types of Testing in a Functional Approach
- Microbiome & Permeability Testing
- These tests look at the health of the gut lining and the balance of bacteria, yeast, and other organisms in the intestines.
- They can help identify increased intestinal permeability (often called “leaky gut”).
- Results can show overgrowths, imbalances, or infections that may be activating the immune system.
- Inflammatory Markers and Autoantibodies
- Blood work is used to track how “active” inflammation and autoimmunity are in the body.
- Markers like hsCRP (high-sensitivity C-reactive protein) help measure overall inflammation. In many functional practices, a common target is an hsCRP level below 1.0 mg/L, when appropriate for the patient.
- Autoantibody tests can help monitor how strongly the immune system is reacting against the body’s own tissues.
- Nutrient and Hormone Panels
- These panels look for gaps that may be quietly feeding the autoimmune process.
- Nutrient tests can check levels of vitamins, minerals, and fatty acids that support immune regulation, energy, and tissue repair.
- Hormone tests may assess thyroid, adrenal, and sex hormones, since imbalances here can influence inflammation, fatigue, and symptom flares.
- History-Driven Trigger Mapping
- This is less about a single lab test and more about a careful, structured interview.
- Practitioners review past infections, major life stress, trauma, environmental exposures, travel, and medication history.
- This timeline helps uncover possible triggers and patterns, which then guide which tests are ordered and how results are interpreted.
By combining these types of testing, functional medicine practitioners can identify key imbalances and more precise targets for treatment. Instead of only tracking whether symptoms are lighter or heavier, this approach follows both how a person feels and how their internal markers are shifting, helping shape a more realistic and personalized path toward remission.
Why Is Gut Healing the Foundation of Autoimmune Remission?
Repairing gut health is central to functional medicine strategies for autoimmune remission. This focus is a core part of functional medicine services for personalized healing, where intestinal integrity is treated as a key regulator of immune balance rather than a separate digestive concern. With approximately 80% of immune cells located in the gut, maintaining a healthy intestinal lining plays a major role in how the immune system responds and adapts over time.
Key strategies for gut health include:
- Elimination Diet Phases: Following the Autoimmune Protocol (AIP) diet can help eliminate harmful inflammatory foods for 4 to 6 weeks.
- Targeted Nutrients and Mucosal Support: Supplements like L-glutamine, zinc carnosine, and bone broth can aid in repairing the intestinal lining.
- Microbiome Rebalancing Tools: Incorporating probiotics, prebiotics, and digestive enzymes helps restore healthy gut flora.
By focusing on gut repair, we can lower immune activation, reduce flare-ups, and create an environment conducive to healing. Once gut health improves, additional therapies become more effective, eventually leading to greater overall health.
Which Triggers Must Be Removed to Sustain Autoimmune Remission?
Continuous management of autoimmune conditions requires removing various triggers from the patient’s life. As part of a functional approach, healthcare professionals look to eliminate inflammatory foods, environmental toxins, hidden infections, and medications that could contribute to relapses.
Some of the common dietary and environmental triggers include:
- Food Antigens and Additives: Common offenders include gluten, dairy, nightshades, and processed sugars.
- Heavy Metals and Chemicals: Toxins from the environment can enter the body and exacerbate autoimmune conditions.
- Hidden Biological Drivers: Conditions like Small Intestinal Bacterial Overgrowth (SIBO) and chronic viral infections must be treated to help relieve autoimmune issues.
By systematically identifying and removing these triggers, we can alleviate the burdens on the immune system, reducing the risk of flare-ups and ensuring long-term remission.
How Is the Immune System Balanced Without Long-Term Suppression?
Balancing the immune system involves using targeted nutrients and modulators to recalibrate the immune signaling pathways without long-term suppression. This is crucial in ensuring patients maintain a healthy immune response while effectively managing their autoimmune conditions.
Evidence-backed immune modulators include:
- Vitamin D: Typical dosing includes 5,000 IU, often aiming for 60-80 ng/ml.
- Omega-3 Fatty Acids: High doses consisting of 2 to 4 grams of EPA and DHA help support anti-inflammatory actions.
- Curcumin: Known for its health benefits, it is often taken as 1g with piperine for improved absorption.
Adjunct therapies, such as low-dose naltrexone (LDN) or peptide treatments, may be introduced to support immune function without the harmful effects of traditional immunosuppressants. These interventions help ensure that the body can respond appropriately to immune challenges.
| Immune Modulator | Typical Dosage |
|---|---|
| Vitamin D | 5,000 IU for optimal levels |
| Omega-3 Fatty Acids | 2-4g of EPA/DHA |
| Curcumin | 1g with piperine, for better absorption |
| Low-Dose Naltrexone (LDN) | 1.5-4.5mg to regulate immune signaling |
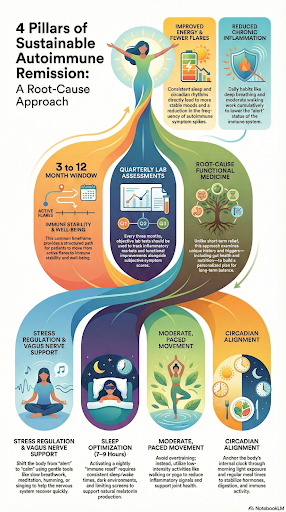
What Lifestyle Interventions Accelerate Autoimmune Remission?
If remission is the destination, daily lifestyle choices are the road you walk to get there. They do not replace medical care, but they often shape how steady and calm the immune system can become over time.
Some of the most helpful areas include:
- Stress Regulation
Chronic stress can keep the nervous system “on alert,” which may keep inflammation high. Gentle, repeatable tools can help shift the body into a calmer state, such as:- Simple breathwork (slow, deep breathing for a few minutes at a time)
- Meditation or mindfulness practices
- Vagus nerve support, for example, humming, singing, or using specific breathing or relaxation techniques
These practices are not about never feeling stressed, but about helping your body recover more quickly after stress.
- Sleep Optimization
Sleep acts like a nightly reset for the immune system.
- Most adults do best with 7–9 hours of consistent, good-quality sleep.
- A regular sleep and wake time, a dark bedroom, and limiting screens before bed can support natural melatonin production.
Better sleep often leads to improved energy, fewer flares, and a more stable mood, which all support remission.
- Moderate Movement
Movement does not have to be extreme to be effective. In fact, overtraining can sometimes worsen symptoms.- Low- to moderate-intensity activities like walking, gentle cycling, or yoga can help reduce inflammatory signals.
- Regular movement supports circulation, joint health, and mental well-being, which are all important in autoimmune care.
Listening to the body, pacing activity, and resting when needed, helps movement become sustainable instead of draining.
- Circadian Alignment and Daily Rhythms
The body’s internal clock affects hormones, sleep, digestion, and immune activity. - Morning light exposure, such as going outside shortly after waking, can help anchor circadian rhythms.
- Eating meals at fairly regular times, winding down at night, and keeping a relatively stable daily routine can support long-term immune balance.
Over time, these lifestyle patterns can create a more stable internal environment, which supports remission and helps prevent frequent flares.
How Is Progress Monitored and Remission Maintained Long Term?
Ongoing monitoring is crucial for sustaining remission in autoimmune patients. Regular assessments aid in tracking key markers and ensuring that the treatment plan remains effective.
Monitoring practices typically include:
- Objective and Subjective Tracking: Utilizing quarterly lab tests helps assess inflammatory markers and functional improvements.
- Expected Outcomes Across Conditions: Each patient’s journey can vary, but benchmarks exist that indicate progress in conditions like Hashimoto’s or rheumatoid arthritis.
Maintaining stable remission often depends on regular check-ins, with adjustments made based on lab results and symptom scores. A timeline of 3 to 12 months is common for many, providing a structured path to immune stability and well-being.
A Root-Cause Path Toward Autoimmune Balance
Some people spend years chasing symptoms without ever understanding why their autoimmune condition began in the first place. That’s where a functional medicine approach can feel different. By looking at root factors such as gut health, chronic inflammation, nutrition, and lifestyle patterns, it offers a more complete picture of what may be driving immune imbalance. From there, it opens a more realistic path toward long-term stability and remission, rather than relying on short-term relief alone.
If you’re ready to explore a more personalized way to manage your autoimmune condition, working with a provider who understands both functional and conventional medicine can be a meaningful next step. Advanced Integrated Health offers health consultations designed to examine your unique history, triggers, and goals, then build a plan that fits your real life and moves at a sustainable pace.
Frequently Asked Questions
How does a functional medicine approach target the root cause of autoimmune disease?
Functional medicine focuses on a root cause autoimmune protocol rather than symptom suppression. It looks at triggers like leaky gut, intestinal permeability repair, dysbiosis, environmental toxin exposure, and hormone imbalance. By restoring microbiome diversity, correcting nutrient deficiencies, and removing inflammatory inputs, the immune system can calm down and move toward long-term autoimmune remission.
What dietary changes support autoimmune remission in functional medicine?
An anti-inflammatory diet for autoimmune remission often starts with an AIP elimination phase. This may include gluten and dairy-free protocols, nightshade-free eating, and sometimes low-histamine or low-oxalate phases. These adjustments reduce immune triggers, calm gut inflammation, and support conditions like rheumatoid arthritis, lupus flares, psoriasis, and IBD remission.
Why is gut healing essential for autoimmune remission?
Autoimmune conditions are closely linked to gut health. Functional medicine prioritizes leaky gut healing, SIBO treatment, and dysbiosis eradication protocols. Support may include zinc carnosine, L-glutamine barrier repair, butyrate short chain fatty acids, and stool testing. Repairing zonulin-driven permeability helps reduce immune overreaction and systemic inflammation.
How do hormones, stress, and lifestyle affect autoimmune flares?
Hormone imbalance correction, adrenal fatigue recovery, and thyroid autoimmunity support are critical for immune stability. Chronic stress raises cortisol and worsens flares, so stress management, HRV training, vagus nerve stimulation, sleep circadian alignment, and blue light reduction are emphasized. These lifestyle changes help prevent lupus flares, MS progression, and autoimmune relapses.
What testing helps guide a functional medicine autoimmune plan?
Functional medicine uses advanced lab testing to personalize care. Common tests include comprehensive stool PCR, GI MAP analysis, food sensitivity testing, DUTCH hormone panels, organic acid markers, and autoimmune antibodies like ANA, TPO, anti-CCP, and rheumatoid factor. Inflammation markers such as hsCRP and ESR help track progress toward remission.

Dr. Bob was born and raised in Florham Park, New Jersey.
He loved the philosophy of vitalism, which teaches about the incredible, innate intelligence of our bodies and its power to self-heal when given the opportunity.